The standout features and strengths of BloodMove are:
- effective communication
- appropriate cold chain security processes
- ongoing education and training
- creating a sense of stewardship and ownership of blood-related processes.
Communication
Communication is ongoing between the BloodMove Team, hospitals and laboratories. In turn, a supportive network is now available that stakeholders can “tap into” – this supports blood management issues. This is particularly important, as BloodMove covers a number of clusters (i.e. regions) across a wide area in regional SA that are supplied by various transfusion laboratories.
Since the implementation of BloodMove:
- existing communication channels have been enhanced and nurtured
- additional communication channels have been established (e.g. communication between pathology laboratories and nominated site contact nurses)
- BloodMove leads have visited sites to provide guidance, training and support to CHSA staff
- BloodSafe clinical nurses meet via teleconference bimonthly; facilitating discussion on blood management
- BloodMove leads provide guidance and support to “hub and spoke” stakeholders; to ensure best practice in blood cold chain management thus minimising waste.
Bianca Strong (BloodSafe Cluster Clinical Nurse) (left) and Sharon Saegenschnitter (BloodSafe Site Contact Nurse) from Kapunda hospital discuss their experience with the BloodMove project in the video below.
If you want to download this video to save it for later or cannot access YouTube download the video from the link below:
Download Transcript:
- Transcript of Kapunda Hospital and the BloodMove Project (pdf) (57.22 KB)
- Transcript of Kapunda Hospital and the BloodMove Project (docx) (21.4 KB)
At times there have been challenges with the BloodMove processes; these minor challenges have been resolved because of the established communication channels and continuous support offered by the BloodMove Team.
Lynda Pierce (HealthScope National Transfusion Coordinator) from Ashford hospital discusses the importance of supportive networks in the BloodMove project in the video below.
If you want to download this video to save it for later or cannot access YouTube download the video from the link below:
Download Transcript:
- Transcript of Ashford Hospital and the BloodMove Project (pdf) (52.9 KB)
- Transcript of Ashford Hospital and the BloodMove Project (docx) (20.34 KB)
Cold chain security
BloodMove ensures that storage, transport and traceability for blood are undertaken in accordance with current standards, guidelines and criteria (see Resources below)
Compliance ensures that supplying laboratories are able to accept blood units back into their inventory for use before expiry.
Existing blood shippers and commonly used packing configuration were validated by BloodMove. Part of this validation involved examination of existing courier systems to identify possible temperature challenges during transport. It was found that the current shipper and transport system utilised were acceptable. BloodMove established that when accompanied with onsite shipper packing education the transportation of blood throughout regional SA would be assured. BloodMove will be providing an independent validation report for the shipper system used throughout SA (i.e. Lifeblood Configuration R1).
When hospital staff are returning blood, it is a requirement that the following are included in the shipper:
- Red Cell Return Form (details blood being returned and confirms that blood was stored and handled correctly whilst at the hospital)
- Copy of Blood Fridge Maintenance Record (evidence of fridge oversight and checking)
- Copy of Temperature Record Charts (e.g thermographs) (objective evidence of storage temperature)
This documentation is used to declare that the appropriate checks have been performed by the hospital whilst storing the blood.

FIGURE: A pathology laboratory staff member prepares a shipper for the transfer of blood
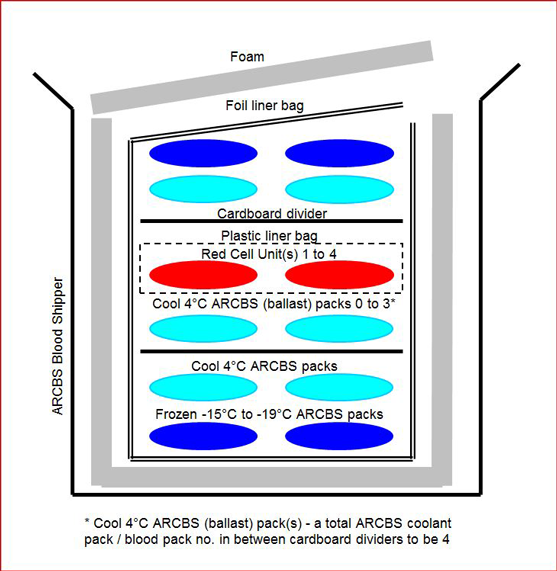
FIGURE: BloodMove Shipper Configuration
All CHSA sites use blood refrigerators that are serviced and used in accordance with Australian Standard AS3864. Blood refrigerator quality assurance is achieved by:
- training staff on how to maintain and use blood refrigerators
- continuous temperature monitoring via thermographs
- regular alarm testing of power loss, high and low temperature challenges and remote activation
- all manual temperature monitoring and alarm tests are recorded on Blood Fridge Maintenance Record.
Tony Waterman (Kapunda Hospital Maintenance Technician) conducts a blood fridge cold temperature alarm challenge in the video below. Please note other alarm challenges are not demonstrated.
If you want to download this video to save it for later or cannot access YouTube download the video from the link below:
- Video - Testing a Blood Fridge Alarm (mp4) (14.97 MB)
Download Transcript:
- Transcript of Testing a Blood Fridge Alarm (pdf) (52.64 KB)
- Transcript of Testing a Blood Fridge Alarm (docx) (20.28 KB)
Andrew Levak, Laboratory Manager, SA Pathology Berri Hospital discusses transport and storage requirements for blood in the video below.
If you want to download this video to save it for later or cannot access YouTube download the video from the link below:
Download Transcript:
- Transcript of BloodMove Transport and Storage Requirements (pdf) (58.38 KB)
- Transcript of BloodMove Hospital Transport and Storage Requirements (docx) (21.11 KB)
All of the above requirements provide assurance to laboratories and hospitals that any blood they are physically receiving has been stored appropriately, can be safely re-introduced to existing inventory and used when required. This is supported and maintained by regular auditing of hospital blood fridge and inventory documentation and processes.
Education and training
A key role of the BloodMove Team is to offer education, training and guidance to the hospital on:
- Accreditation and compliance with applicable standards and guidelines
- Correct storage, transportation and handling of blood
- Correct completion of all documentation
- Emphasising the need to report blood management incidents into the SA Health Safety and Quality incident database
- Administration of blood and blood products to patients
- Nurturing blood stewardship and respecting this valuable donated product.
This is an ongoing process that is standardised across all hospitals in accordance with best practice.
Stewardship and ownership
BloodMove has achieved a cultural change across regional SA on important issues such as blood-related costs, inventory management and minimising avoidable blood wastage.
The change has been brought about by the education provided by BloodMove site visits detailing the sense of blood stewardship and ownership in their duties whilst the blood is in their possession. CHSA hospital staff and transfusion laboratory staff now are mindful of any blood wastage and question and attempt to resolve all causes whereas in the past such wastage was accepted as unavoidable.
BloodMove has become part of normal accepted practice at sites across country South Australia. A recent highlight for the BloodMove Team and for all stakeholders was that there was only one (1) blood unit being wasted in the whole of regional SA in February 2013. The Team even investigated that one, to see what could have been done to prevent it.